Sunday, September 15
9:30 pm
“This is the first night that we are going to sleep and I am not confident that we are going to make our due date.” This is what I said to Lyndon three and a half hours before my labour began. Call it mother’s intuition? Because there were no glaringly obvious signs that our babe was about to make his entrance. Lyndon responded rather indifferently to my remark and we said our usual “good night/I love you’s”.
Monday, September 16 (38 weeks pregnant)
1:00 am
POP.
I woke up instantly to what I can best describe as a “popping” feeling inside me. ‘Don’t waters go “pop” when they break?!’ I thought to myself in the dark. I moseyed out of bed and to the bathroom. No movie-esque gushes. Probably nothing. Except for that it wasn’t nothing. I will spare you the TMI details but there were some signs that labour may just be beginning. Now the problem with labour is that these TMI type things can happen a few weeks prior to labour, or a few hours prior to labour. If you’ve ever had a child in the time of Google, you will also know that all of your symptoms can seemingly either be a sign of false labour or true labour. I still don’t understand this distinction. Nonetheless, what started as a mild lower backache transformed into an intermittent cramping feeling. Contractions had begun.
1:45 am
I poked Lyndon.
Me: “Lyndon… I think we might have this baby.”
Lyndon (sleepily): “Really? Then we should probably get more sleep.”
Ummm… easy for you to say. He rolled over and with a comforting pat and left me to my own devices. Fair enough, as at this point, I was unconvinced that this was even happening (clearly, he was too). I downloaded a contraction counter app just in case, laid in the dark trying to relax in between these crazy cramps, and started timing them when they showed up.
2:00 am – 4:00 am
1:5:1 – This is what they taught us in prenatal class. When contractions are one minute long, five minutes apart, for one hour, it’s ‘go to the hospital’ time! Mine were sporadic… most were about seven minutes apart but sometimes I would go ten or eleven minutes in between. I was told multiple times that having a first child is a slow process, so I assumed we had all the time in the world and concentrated on recalling my “labouring positions”.
5:00 am
I poked Lyndon again.
Me: “I think we should get up and pack our hospital bag.” (Good thing I am the farthest thing from a procrastinator and the bag was mostly packed despite being two weeks away from our due date).
Lyndon: “Really?” I showed him my contraction counter and we analyzed the pattern. “We should go to the hospital!” he told me.
Me: “Nahhh…. This is supposed to take forever and it doesn’t hurt enough yet [I say as I’m doubled over not able to talk for minutes at a time].”
I assumed that I must be in absolute excruciating unbearable agony before it would be time to go.
Me: “Let’s make breakfast!”
We eat bacon and eggs. Lyndon makes French press coffee. Every couple of minutes I hunch over the kitchen stool and breathe through another contraction. Lyndon attempts some of the comforting tactics we learned in prenatal class (i.e. touching me).
Me: Don’t touch me!!!
I set myself up in the nursery with my exercise ball preparing myself for a long day of labouring. I distinctly remember what happened next.
Lyndon: Well, I need to go to the bathroom!
He heads to the other end of the house and the bathroom door closes.
GUSH.
OMG. There it is. The movie-esque dramatic water-breaking scene.
Me: AHHH! LYNDON! I’M GUSHING!!!
Lyndon (from the bathroom): WHAT?!
He rushes back out to find me bow-legging it to the bathroom trying not to leak fluids all over the floor. Lucky for me, two of my trusty friends who had been through this before had shared a little nugget of wisdom only a few days prior: the convenience of having Depends disposable undies on hand! I left my dignity in the puddle and pulled those babies on! Now what they do not show in the movies is that rather than one large gush, it is more of a continuous gushing situation with every move you make. Also, my contractions intensified. This may have been the point that I accepted the reality of the situation. Our baby was coming. Today. Lyndon loaded the car in a hurry and I waddled out.
7:00 am
The ten-minute car ride seemed to take forever. With every bump, I moaned in agony and I tried to ride through the contractions while buckled in my seatbelt.
We arrived at the hospital and I dripped my way into the elevator that took us to the maternity ward. We reached the check-in desk and the nurses ushered me over to the ‘you don’t need to wait in line’ spot. I responded to this act of kindness by grabbing the nearest garbage can and throwing up my entire breakfast while crippled over the desk.
The nurses took me to an assessment room where I stripped down.
Nurse: Has your water broke?
I pulled my diaper off and it thunked to the floor with its weight.
Nurse: Yup! Your water definitely broke!
She did her assessment (the first of many fun things to come).
Nurse: You’re six centimeters already!
My jaw dropped. Six centimeters?! This was supposed to take all day! I silently applauded my body for being speedy about things! Maybe this labour/birth thing wouldn’t be as traumatic as I anticipated?!
We were brought straight to delivery where I was asked if I wanted an epidural. Now at this point, if things would have stayed the way they were, I think I could have managed but I had the wherewithal to know that things were going to get much much worse, so I opted for that epidural ASAP. Lucky for me, I was told that I was next in line so I didn’t have to suffer through the worsening contractions for much longer. In the meantime, our lovely nurse got my IV going.
About half an hour later, the goddess that is the anesthesiologist walked in with her epidural magic. This sweet doctor ran through the risks and through gritted teeth I told her that yes, I indeed still wanted the epidural! Despite the pain, however, my brain did not forget about my withstanding fear of death-by-allergy to something in the numbing concoction. I quickly regaled my recent unexpected allergic reactions (see previous blog post for details of this fear) and the doctor made a worried face: “This concerns me.” Oh no. By bringing this up did I just doom myself to an unmedicated birth?! This was not in the plan. The doctor left the room momentarily to do a bit of research and returned declaring that she thought it would be okay to go ahead with it. Thank goodness. She did, however, decide to go easy on the medication just in case.
For those who may be reading this in a pregnant state, I am happy to report that actually receiving the epidural was not nearly as terrifying and/or painful as I expected! The procedure went smoothly despite having to stay still during a few contractions while they inserted the needle. Fifteen minutes later, the contraction pain had subsided to a very manageable level and I felt like myself again!
Suddenly, I was a chatty Kathy! We got to know our sweet nurse, met our resident doctor who was an equally lovely young man, and my own family physician arrived to assess the situation. When she walked in, I was happily eating a Popsicle, snapping a selfie of Lyndon and I, and texting our close family and friends that we were going to have a baby today! My doctor told me that she would check me, then go to her office for a while and come back when it was go time.
9:30 am
She checked me. “You’re 9.5 centimeters!” My jaw dropped for a second time. WHAT?! You mean I’ve gone through literally everything already and it’s almost time to push this baby out?! I honestly thought in this moment, if all my labour experiences were like this, I could do this again! “I guess I’m not going to my office!” my doctor remarked. “I think you’re going to have this baby by noon!” the resident told me with a smile! The doctors told me that soon, I would feel an urge to push and then we could have this baby! I was elated.
So we waited. And we waited some more. In the meantime, I started feeling my contractions a little more than I had hoped to, so we got the anesthesiologist back in to top up my epidural, as I had clearly not died of an allergic reaction. Once again, the pain subsided… but this time, perhaps a little too much so. I felt nothing. In fact, I could literally not move my left leg. I was no longer able to get up and move around as I had no use of my lower half, thus, a catheter was required for bladder drainage purposes. I did not like the sound of this, but quickly realized it mattered zero when ten minutes later, I asked if it was in and they all looked at me funny and said it was in and out ten minutes ago. Huh.
12:00 pm
“Do you feel an urge to push?” the resident asked me after a few hours of waiting. “Nope,” I replied, still in my blissful state of frozen. My doctor checked me again. “You are ten centimeters dilated and I can see the baby’s head… It’s ‘right there’… are you sure you don’t feel an urge to push?” I was baffled. Did I? I checked in with my body. Nope… I really didn’t. “Alright, we are going to do some test pushes anyway,” I was told by the team. Okee dokee then, let’s do this. They wrapped two monitors around my tummy, one to monitor the baby’s heart rate and another to measure my contractions. Based on the readings, I was instructed when to push. And push I did. In fact, they made me feel like a pushing rock star! “GOOD JOB, AMANDA! THAT WAS A GREAT PUSH! YOU’RE DOING SO GOOD!” The medical team chanted excitedly every contraction. In hindsight, it has become clear to me that they pump every woman up this way, but it definitely worked in the moment. I felt empowered and I was ready to deliver this baby!
Except for that my body apparently wasn’t ready to deliver this baby.
First, during several of my contractions, a decrease in heart rate was observed in Baby E. The team told me that it is possible that the umbilical cord was wrapped around his neck. This scared me a great deal, but their presented sense of calm in regards to the situation helped me remain calm as well.
Second, after about an hour of “great” pushing, the team could still see the hair on the top of Baby E’s head that they claimed to see at the top of the hour, however, said hair was no closer to being earthside.
Third, my contractions slowed down. And then slowed down more. And then slowed down to the point that we were waiting around for ridiculously long stretches of time in between bouts of pushing and the resident started yawning so Lyndon offered to get him a stool. How gentlemanly.
A team of four from the neonatal intensive care unit arrived and stationed themselves at the back corner of the room awaiting Baby E’s arrival, gloved and ready. I thought it was funny that they didn’t acknowledge me or anyone else in the room so I gave them a wave and said, “Hello, peanut gallery!”. They barely but smirked in response. Alrighty then, I’ll go back to the task at hand.
I was given oxytocin to start things back up again. And it worked! Until it didn’t. They gave me another round of oxytocin. With every round of pushing, Lyndon quietly whispered, “Push, push, push, push, push, push…” ‘What do you think I’m doing?!’ I thought to myself. I mean, thanks for the encouragement, babe! 😉
3:00 pm
Baby E’s heart rate was rising. I had been pushing for three hours. I was exhausted and the team told me it was time to get the baby out. A second nurse arrived to assist with the delivery. We now had eight medical team members present. My doctor pulled out “the vacuum”. I recalled a vacuum horror story a friend had recently shared about her own delivery (as well as everything I had read about head injuries due to instrument use during delivery) and adamantly told my doctor that I did not want the vacuum… or forceps. The team looked uneasy and let me try a few more pushes. When that failed, they presented the idea of an episiotomy. Again, I will spare you with the details of that lovely procedure (Google it if you’re so inclined) but I quickly agreed to go ahead with it. My motherly instincts were already intact. I knew immediately that when given the choice, I wanted to go that route because I would rather hurt myself than put my baby in jeopardy in any way.
The doctor did what he needed to do. Two pushes later, the resident said, “Do you want to feel his head!?” “NO!” I squeaked breathlessly… ‘I have my whole life to feel his head, let’s get his body out of here!’ I thought to myself. Lyndon later shared that when his head came out, the resident quickly and smoothly grabbed the cord, unwrapping it from around baby’s neck and continued the delivery without a hitch. Two more pushes, and I heard, “He’s out!”. Oh my God. He’s out. He’s here. I did it. Lyndon cut the cord. They put my gooey little man on my chest and I felt overwhelmed with emotion. Tears rolled down my face as I tried to comprehend that this tiny human that grew inside of me for nine months was actually here.
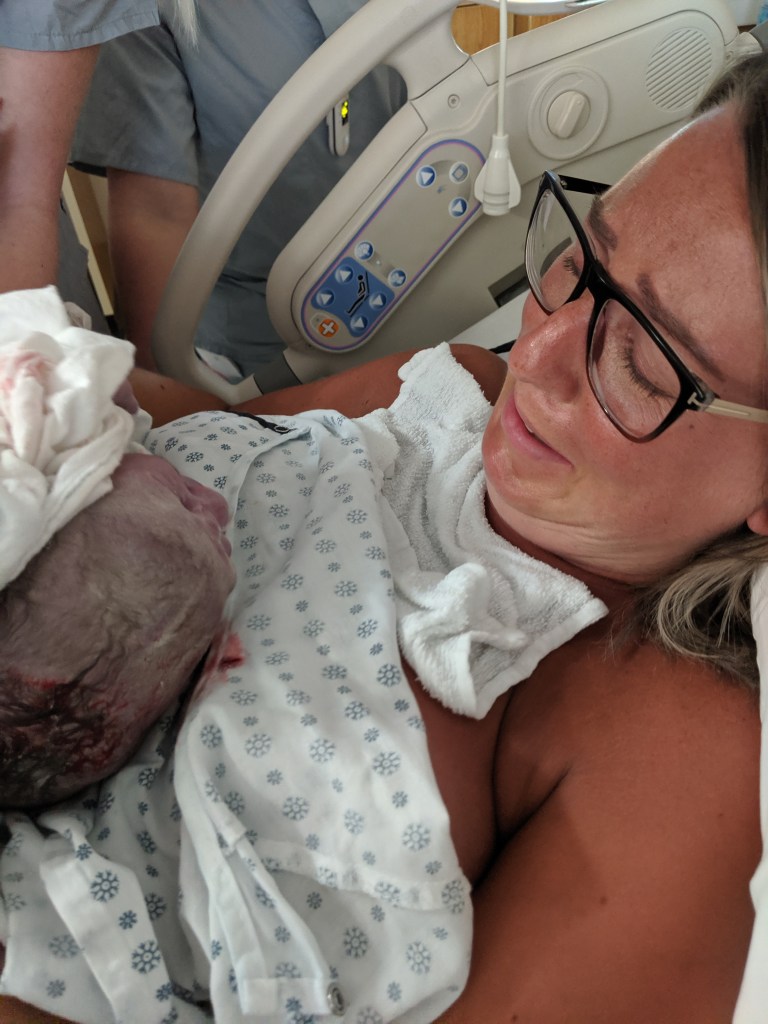
I was ready to breathe that huge sigh of relief that everyone assured me was to come when I met my baby.
I would love to say that is what happened next.
Sadly, it is not.
Instead of having an hour of skin-to-skin time with my baby son, and attempting to establish a breastfeeding latch within the first hour (i.e. my best case scenario going into delivery) my baby was whisked off my chest within a couple minutes and taken to the corner of the room to be examined by the NICU team. I stared across the room and listened to my baby cry. What is happening?! Lyndon went with the NICU team to observe their examination. “Is he okay? Is my baby okay?” I cried.
Lyndon didn’t respond.
My heart sunk.
“Is everything else okay?” I demanded from the bed where I was stuck.
Lyndon looked at me and gently told me that there was something different about our baby’s foot.
I felt like my heart ripped in two. I thought about how the genetic counsellor said that there was a nine out of ten likelihood that our son’s hand was an isolated incidence. We were the “one”. Again. I wanted my baby back so I could see him with my own eyes. “We’ll get him cleaned up and then we’ll take a look at him together,” my doctor told me kindly.
They brought our boy back following the assessment and he laid on my chest while the doctors did what they needed to do to patch me back up. “Does he have a name?” the team asked. Cade Brooks Ellis. He has had a name since conception. He has always been our little Cade. “That’s a good, strong name,” someone commented. I agreed.
Our doctor unwrapped Cade and I got to see his “lucky fins” (plural) for the first time. His left hand looked much like we expected. He had two digits, one that looks like a thumb in the position of a finger and one finger. But the digits were not fused as expected which is positive. If I am honest with myself, seeing Cade’s lucky fin for the first time is a moment that I feared. I worried what my genuine reaction would be and if it would be appropriate (whatever that may be). I truly don’t know how to describe how I felt seeing his unique little hand. It just was. It was a uniquely perfect little baby hand on my uniquely perfect baby. The doctor unwrapped his foot. My first thought was that it looked like he has a little flipper. His foot was flexed so that the top of his tiny foot rested on the top of his tiny leg. He had four little toes, all of which were webbed together. Again, it just was. Uniquely, Cade.


And then there was the rest of him. His adorable little face, his soft dark hair, and his smooth baby skin. He was intoxicating. My heart burst with love for this little man. I knew in the back of my mind that our journey was not about to get any less complicated. In fact, especially with the discovery of his foot, I knew that our boy was going to have many mountains to climb moving forward. But these are not the things that I dwelled on in the next few hours. I simply loved on my adorable, baby boy.
He is here and our adventure has only just begun.
To be continued…

Congratulations on the birth of your beautiful baby boy…..love your blog….❤️
LikeLike
That is the most beautiful story I have ever heard. As equally as beautiful as you. Congratulations!!!!
LikeLike
Congratulations! He is beautiful and your family is adorable!
LikeLike
Congratulations…he is beautiful! I will let everyone know here, I enjoy your honest genuine blog….you are both beaming! You are a natural mother ❤
LikeLike
Welcome to ther world baby Cade!!!! Congratulations you guys and Wishing you a smooth recovery Amanda!
LikeLike
Such a beautiful love story. ❤️ What a wonderful family! Congratulations, and well done Mama!
LikeLike
This was such a beautiful story, thank you for sharing. He is absolutely adorable.
LikeLike